My 2025 drew to a close with the salty breeze against my skin and the grit of wet sand between my toes, walking along the beach at sunset.
And then…ouch…what was that?
I lifted my foot expecting to find a shell, only to see a small black stinger stuck in the middle of the sole of my foot, complete with pulsating sacs of venom. On the ground nearby lay the poor little bee who had his dreams of seeing 2026 cut sorely short.
“Sorry, my bee friend” I chirped sweetly, like Cinderella communing with the birds in a Disney cartoon.
That’s untrue. I jumped around ungainly swearing my head off as the toxins deposited beneath my skin, activating my sensory system.
Thankfully I don’t get anaphylaxis from bees (RIP Thomas J in My Girl, I will never recover from that movie inflicted grief). However, just over 24 hours later my immune system let it’s presence be felt as my foot screamed “itch me” in the dead of night.
For three days and three nights(ish) it lasted. The centre of my foot remained flushed pink by the blood vessels carrying in the inflammatory mediators and immune cells to disarm the bee venom molecules and eliminate them from my body, leaving nothing but an inspiration for a post behind.
Nature’s drugs and delivery systems
Bee venom is a mix of chemicals including peptides (short chains of amino acids), enzyme proteins (long chains of amino acids), and amines (small molecules like histamine). The specific details of the components don’t really matter for the purposes of this post. What matters is that bee venom is an exogenous substance that is able to exert an effect within the body, meeting the Lessons on Drugs broad definition of a naturally occurring drug substance.
As we’ve talked about in previous posts (like bodily logistics and the caffeine as a gateway drug series), the first thing that needs to happen for a drug to exert an effect in the body is for it to get to where it works.
Most naturally occurring drugs get into the body by being eaten, but animals like bees, snakes, and spiders carry their own drug delivery system [insert mental image of a bee in a nurse’s outfit here]. The bee’s stinger acts like a hypodermic needle. It may only be around 2mm long, but long enough to pierce it’s way through the skin of an unsuspecting animal. Once it’s lodged, their little venom glands take the role of the plunger in a syringe, forcefully injecting venom into their victim.
If you think that sounds a bit brutal, it’s because it is. As I’ve explained before, all injections result in some degree of physical trauma to the body - like entering a building by breaking through a window rather than using the front door.
The good thing about bee venom is that unless we’re talking about some sort of Teenage Mutant Ninja Bee, there are natural constraints on how much can be administered, and where in the body it will end up. To liken it to a pharmaceutical product, the venom composition can be thought of as the formulation, where the venom sacs determine the vial size, and the stinger the gauge and length of the needle.
So let’s take a moment to consider another naturally derived drug that’s purposely administered into the skin…Botox.
Botox is a brand name for a purified and heavily diluted formulation of the highly potent and fatal botulinum toxin, a naturally occurring toxin produced by a bacteria called Clostridium botulinum.1 Unlike bees, Clostridium botulinum didn’t evolve to have inbuilt syringes to inject their highly potent and lethal toxin into unsuspecting animals (phew!).
Whilst naturally occurring botulinum toxins still make their way into humans via contaminated food on occasion, it most commonly makes it’s way into millions of humans across the world through needles, held in the hands of what I hope are well trained professionals. Because when it comes to determining the exact dose of toxin administered, where it ends up, and the effect it has on the body, well that’s where product preparation and administration technique matter.
To explore this, let’s turn our attention to the biggest and possibly most underrated organ in the body…the skin.
What do we mean by ‘skin deep’?
The skin is structured in three major layers that we’ll consider from the outside in, illustrated in the figure below.
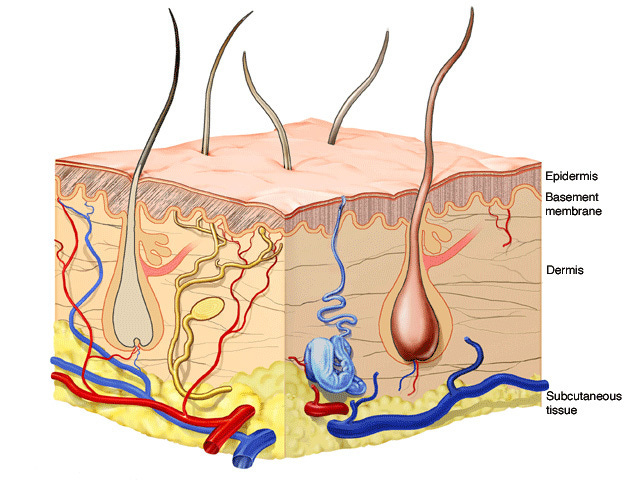
The thin outer layer is called the epidermis. It’s the ‘protective coat’ that prevents unwanted things getting into the body, keeps the wanted things inside, and provides the exit point for things like hair, sweat, and sebum to maintain the living conditions for all the microbes that make our outer surface their home. This layer doesn’t contain blood vessels - it receives its nutrients and has waste removed from interactions with the layer below.
The thick middle layer is called the dermis which gives the skin its structure through fibres like collagen and elastin. It houses the sweat and sebum glands (pimples!), hair follicles, and has infrastructure like nerves, blood and lymph vessels passing through.
The third innermost layer is the fatty subcutaneous tissue or hypodermis which also contains nerves, blood and lymph vessels. Oh, and fibrous connective tissue called septae which can give rise to cellulite for those who are blessed. This padding helps keep us warm and protect our body from the brute forces of the outside world.
Below the skin, you’ll find the fascia, muscles, bones, and internal organs - a further journey in some places than others. Which brings us to consider the importance of injection administration technique.
As I’ve illustrated in the artistic masterpieces below, it’s feasible that stepping on the poor little honeybee could have penetrated all layers of skin if the angle was right, owing to the anatomy of that particular part of my foot. If I sat on the bee however, I can say with confidence that the stinger would not have been long enough to pierce all three layers of skin regardless of the angle of entry, owing to the considerably thicker subcutaneous layer.
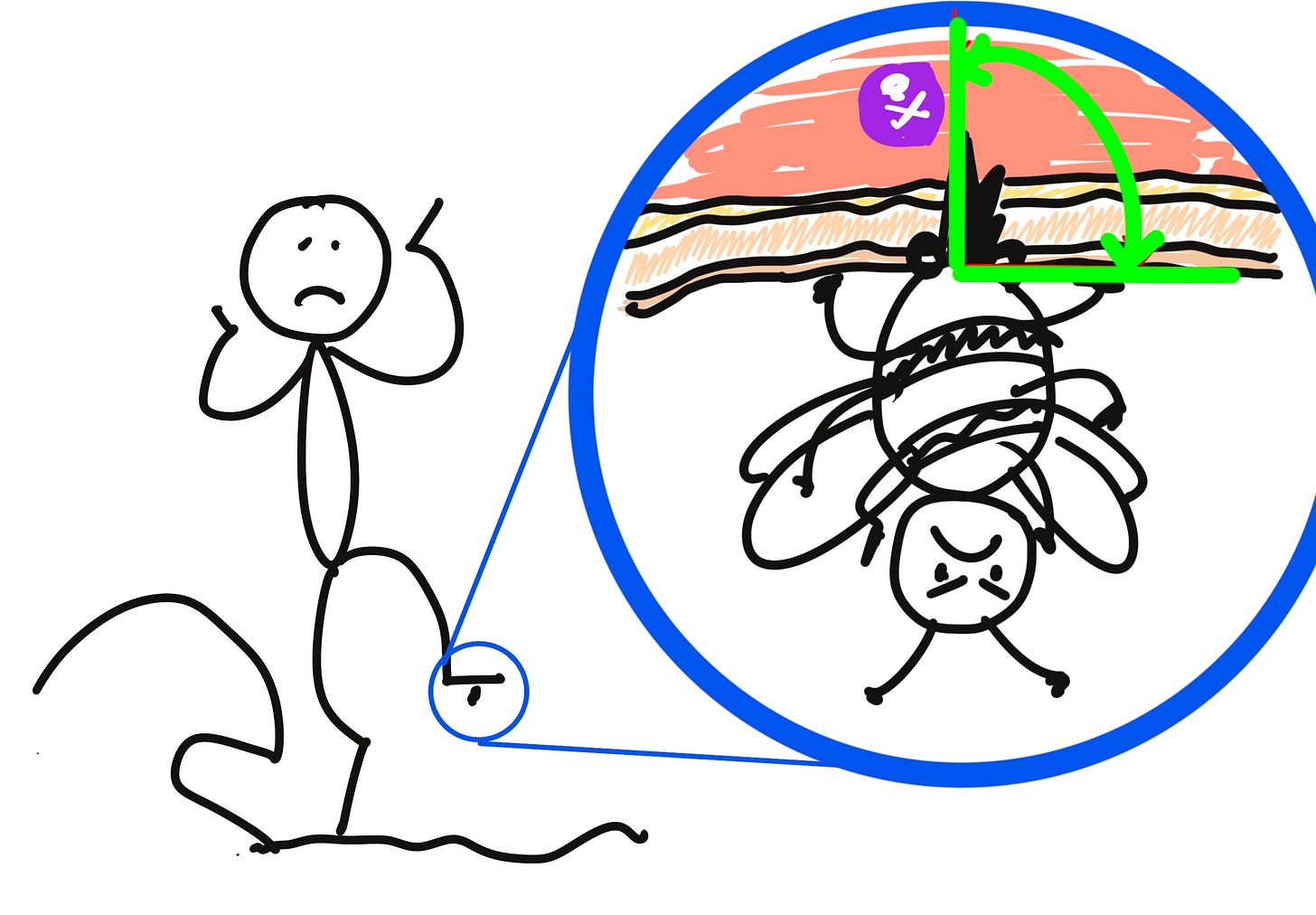
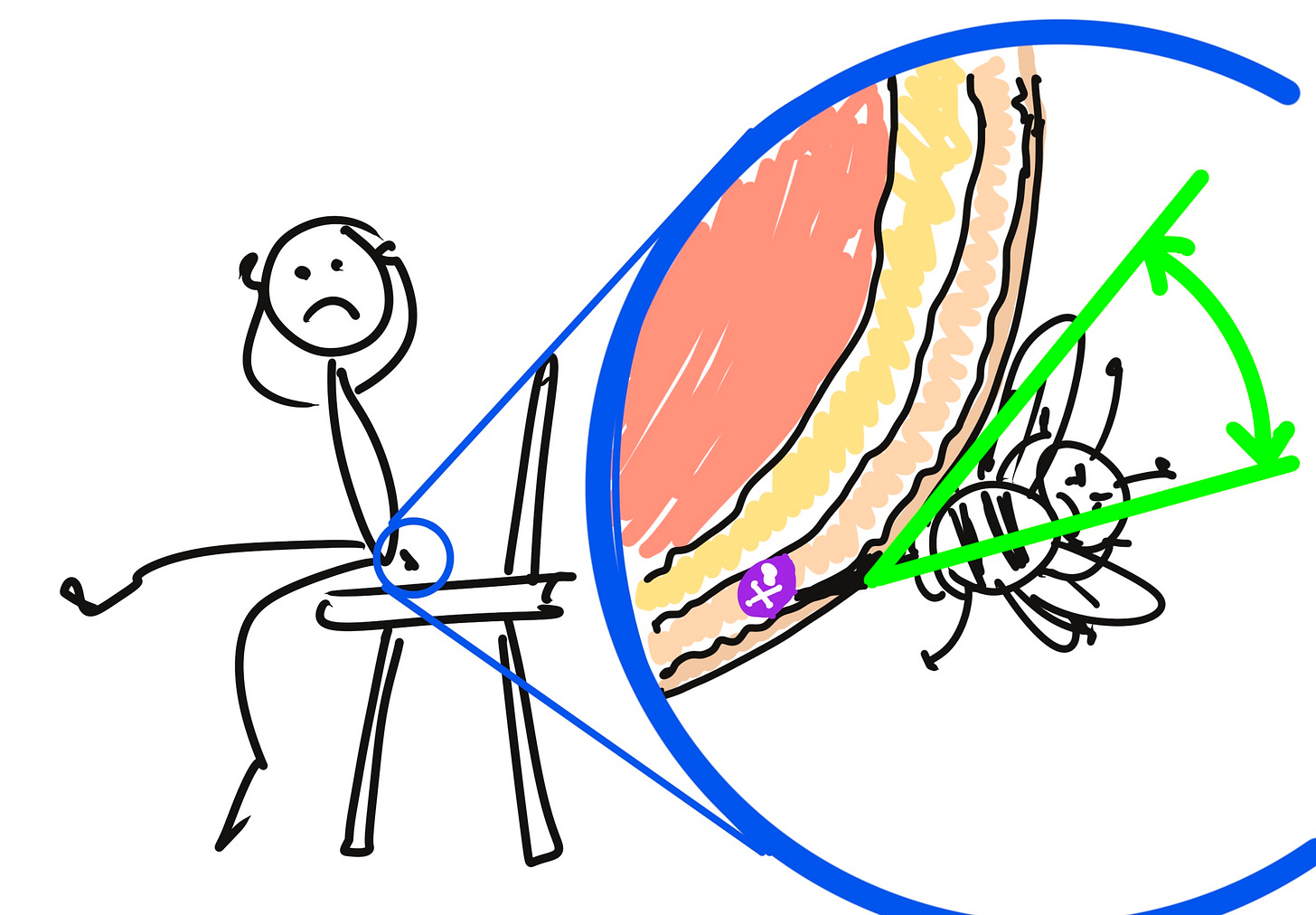
These basic principles - geometry combined with knowledge of anatomy - are applied when pharmaceutical products like Botox® are injected through syringes held by human hands.2
The dose makes the poison
Botulinum toxin works by blocking nerve cells from releasing acetylcholine, the main neurotransmitter involved in the voluntary movement of muscles (somatic nervous system) as well as the ‘rest and digest’ type involuntary bodily functions that keep us alive (the autonomic division of the parasympathetic nervous system).
When it comes to banishing dynamic wrinkles, the most common use of Botox,3 the goal is to stop specific facial muscles from contracting and pulling on the skin. The problem is, the drug doesn’t differentiate between nerve cells - it will happily enter whatever nerve cell is in proximity and stop that cell from sending signals, whether those signals are destined for the desired facial muscle or not. The only way of avoiding this is through it being given by a responsible practitioner who is able to carefully place just enough drug in just the right place.
With regards to the ‘just enough drug’ part, this is where sticking with licensed products and approved dosing regimens is important. This is not a ‘more gives better results’ situation. And definitely not a ‘see what I can get through Amazon’ type purchase. I did mention it’s a potent neurotoxin, right?
As for the ‘just the right place’, well this can be tricky. It’s not like putting a dose of vaccine into the deltoid muscle of the upper arm where there’s a reasonable margin for error. The muscles of the face are close together and overlap, with exact placement varying from person to person. Targeting the neuromuscular junction precisely requires a skilled practitioner with steady hands.
Disarm you with a (temporarily wrinkle free) smile
Most of the drugs we’ve looked at in other posts are relatively simple molecules that interact with receptors found on the outside wall of a cell and move around the body and into the bloodstream to varying degrees.
Bee venom and Botox are much bigger chemical structures - bee-tox is a mixture containing peptides (short chains of amino acids), while Botox is a protein (long, folded chains of amino acids). Because of this, they don’t move easily from where they’re injected unless something actively transports them.4
In the case of Botox, the nerve cell opens the door and welcomes it in the form of a vesicle, which is kind of like asking a vampire to come to dinner. Once inside the nerve cell, the Botox becomes activated, unfolding its light chain to waggle away in the cytoplasm. Here, it acts as an enzyme, disrupting the nerve’s usual process of releasing acetylcholine.
If you’ve ever done any chemistry, you’d be familiar with the word ‘enzyme’ - a substance that enables a chemical reaction to occur, but doesn’t get used up in the process. It’s this feature of Botox that makes it such an effective neurotoxin - it continues to have an effect within the cell until something disarms it. This takes time.
Gradually the nerve cell breaks down the Botox molecule through its usual degradation pathways, chopping up the protein into its amino acid building blocks. At the same time, the nerve cells do some remodelling, and over a few months neurotransmission (and muscle movement) gradually returns.
But that’s not the only way your body gets rid of toxins like Botox and bee-tox - it also has the immune system, in which our skin plays a major role.
The killer in me is the killer in you
As the outermost layer of our body that comes under constant attack from potential pathogenic invaders, it’s not surprising that our skin comes armed with its own regiment of soldiers ready to be mobilised on short notice. Yes that’s right, those top two layers of skin don’t just house sweat and sebum, there are also a bunch of immune cells ready to spring into action [insert mental image of a neutrophil dressed like an SAS officer lying in hiding with a machine gun here].
In addition to the white blood cells, the skin has other immune cells to help actively kill off invaders, sound the alarm and open the gates to bring in reinforcements, and instigate targeted missions to take down enemies it’s dealt with in the past.
What I’ve loosely described above is the innate immune response (including inflammation), and the adaptive immune response. To explore this further let’s return to the bee.
When that little bastard bee pierced my skin, it triggered a reaction in my body before my body even understood what chemical weapon it had been hit by. When we looked at the structure of the skin earlier, I mentioned that the top layer doesn’t contain blood vessels, which is very useful for an intact defensive layer but less useful when it’s been damaged, because that layer needs to be repaired, pronto. And so, my body quickly opened up the blood vessels in the deeper layers of skin and tissue (vasodilation), making the area area look pinker.
What I couldn’t see from the outside was the local immune cells springing into action gobbling up what venom they could (phagocytosis) and sending off their alarm signals (inflammatory mediators like cytokines and histamine) to bring in the defensive reinforcements (immune cells). I did start seeing evidence of this later though, as the area around the sting started to swell and get itchy as the defensive reinforcements moved from the blood vessels into the tissue surrounding the intruder.
It’s important to note that the very act of penetrating the skin triggers this innate immune response,5 not just the administration of drug substances. Any type of injection exposes our body to risk of infection and the need to heal itself. We can help reduce the inflammatory response by taking actions that reduce blood flow to the area, like applying a cold pack, avoiding strenuous exercise and other things that promote blood flow (like alcohol). In the case of a drug like Botox being injected, these actions also help reduce it moving into other nearby tissues and causing unwanted effects.6
So that’s an overview of what happens with the innate immune response, now let’s turn our attention to the adaptive immune response. I’ll have to save the details of this for another post, suffice to say that the adaptive response is concerned with the ‘long game’ actions that enable our immune system to learn about invaders and devise plans for future attacks. It does this through the formation of antibodies (immunoglobulins).
Some people form the type of antibodies (IgE) that cause their body’s defenses to go overboard, resulting in an allergic hypersensitivity reaction or in some cases, a life-threatening multi-system reaction called anaphylaxis. Other times, the types of antibodies formed are more moderate in their actions, priming the body to respond to an invader quickly and reducing it’s effects. This type of acquired tolerance or immunity can occur with both bee venom and Botox.
For a bee keeper, developing tolerance to bee stings is a good thing, but for someone paying hundreds of dollars for Botox injections I imagine it’s not so great. Yet another reason why, if you’re going to use it, you should use the smallest amount possible.
Thanks for reading Lessons on Drugs! If you got this far, please think about hitting the like button, sharing a comment, or sharing the post with others.
And for the song reference and some nostalgia…
There are other brands available and they’re not all immediately interchangeable, but I’m using Botox as an overarching term. Anyone know the term for when the lead brand like Kleenex or Band-Aid is used to describe all the products in that category?
General rule of thumb angles are used to guide administration of vaccines- 90 degrees for intramuscular, 45 degrees for subcutaneous, 5 to 15 degrees for intradermal.
Botox is also used therapeutically for indications like overactive bladder, spasticity, migraine, and excessive sweating.
There is some evidence that Botox is actively transported by neurons through axonal transport, allowing the molecules to move further away from the injection site. It’s thought this is more likely at higher doses and is unlikely to cause any problems at the small doses used cosmetically.
Another commonly encountered example of this is tattoos. The process of tattooing involves droplets of ink being injected into the middle layer of skin (dermis). The body reacts initially in the same way as it does with the bee sting - opens up the blood vessels and activates the local immune cells who try to gobble up the ink.
For most people, this causes some mild swelling and redness that goes away after a few days, and slight fading as the immune system gobbles up a few of the smaller ink droplets. But occasionally people experience other immune-related responses, like a flare up of an inflammatory skin condition or autoimmune disease, or an allergic reaction. There’s been some interesting research come out about the relationship between tattoos and the immune system recently, but it’s still too early to draw conclusions about what this means for people in real life.
One aspect of the immune system we do know is very relevant to tattoos though is in regards to laser tattoo removal, which relies on the body’s immune system to do a most of the work. Lasers are used to break the ink droplets down to a size small enough to be internalised and destroyed by immune cells through phagocytosis. This is why it takes multiple sessions and response varies between individuals.
As someone living in Australia with a bunch of venomous snakes, spiders, and sea creatures, I feel a responsibility to mention that reducing mobility is potentially life saving first aid.
Pressure bandages are best for snake bites, funnel web spiders, blue-ringed octopus, and cone shells, but should not be used for other spiders, jellyfish, or insect bites.




Fascinating stuff Lauren.
“To get through the ample cushioning of my bee-hind.” Ha!
Great post!